What We Do
CDIMD's primary mission supports the clinical integrity of ICD-10-CM/PCS codes that must be based upon provider documentation of terminology mandated by the ICD-10 Cooperating Parties (which is not necessarily the same as what physicians read in their literature), a process known as clinical documentation integrity (CDI) or clinical documentation and coding integrity (CDCI).
By engaging CDIMD, hospitals and physicians promote AHIMA's and ACDIS's industry standards of having a coding or CDI escalation policy when documentation does not fit the clinical circumstances or if there is disagreement on how an encounter should be coded or sequenced.
While we specialize in physician, clinical, and coding DRG, HCC and ICD-10 training and support (prospective, concurrent, and retrospective environments), we differ in that we avail our expertise and experience on an ongoing basis, especially in an urgent pre-bill environment, when there is concern for the clinical validity of a provider documentation or disagreement on how ICD-10-CM/PCS codes should be assigned or sequenced.
Many of our clients have had relationships with other consulting firms for training of their concurrent reviewers (e.g. 3M, Huron), implementation of computer-assisted coding and physician query programs (e.g. Nuance, Optum), and installation of tracking software (e.g. Midas, CDIS, Chartwise). They rely on CDIMD on an ongoing basis to address immediate challenges in assuring the clinical validity of HIPAA-transaction sets or developing/maintaining their own physician champions, coding, and CDI staff.
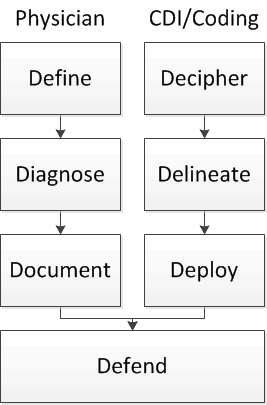
CDIMD supports the interdependent CDI relationship providers and coders must have if accurate code assignment is to be achieved.
We understand each entity's responsibilities and help bridge the gap.
